Osteoarthritis is perhaps the most recognised form of arthritis, which affects the whole joint including the bone, cartilage, ligaments and muscles.
The chance of developing osteoarthritis increases considerably after the age of 45.
There are more than one hundred types of arthritis. Each type affects the joints in different ways and the degree of pain experienced will vary between patients.
With its prevalence on the rise in Australia it is essential that you know how to recognise and respond to arthritis in your practice.
Osteoarthritis is a condition resulting in pain, swelling and/or reduction in motion. Like other forms of arthritis, osteoarthritis tends to worsen over time.
As the condition progresses, everyday tasks that were once simple can become a challenge.
Initially, a person will experience pain during and after physical activity, but as the condition progresses pain will be present during minor movements or even while resting.
Socioeconomic factors influence the chance of a person developing osteoarthritis.
A recent National Health Survey conducted in Australia found that people living in lower socioeconomic areas had a prevalence rate of 26 per cent compared to 16 per cent for people in higher economic areas.
In addition, from 2005 to 2017 there was a 38 per cent increase in the rate of total knee replacements as a result of osteoarthritis.
What is osteoarthritis?
© Inflammation to the tissues around the joints;
© Cartilage tear/damage;
© Bony spurs growing around the edge of the joint; and
© Ligament deterioration.
Osteoarthritis can affect any joint. However, it occurs most often in;
© Knees;
© Hips;
© Finger joints; and
© ‘Big’ toes.
Symptoms
The following is a list of common symptoms (bear in mind that symptoms will differ depending on the joint affected):
© Stiffness and pain in joints;
© Crepitus: clicking noises, grating sensations, crunching sensations (crepitus);
Who is most at risk of osteoarthritis?
© People who have a previous injury;
© People who are overweight or obese;
© Older people;
© People who have joint misalignment;
© People who work in roles that require repetitive tasks that put strain on joints;
© People with a genetic disposition to osteoarthritis; and
© Women are more likely to develop osteoarthritis than men.
Diagnosis
A doctor will diagnose osteoarthritis from a combination of a patient’s symptoms, their medical history, and a physical examination.
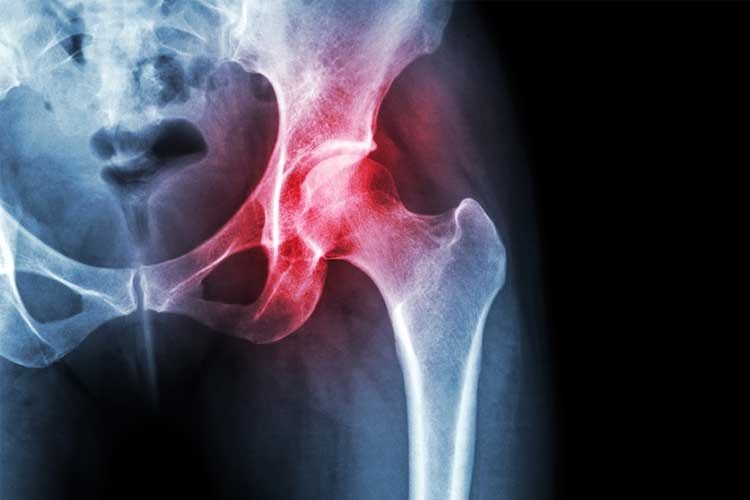
An x-ray might show the narrowing and changes in the shape of the joint, however, an x-ray may not be enough to demonstrate how much pain a patient is in. Blood tests will only rule out other types of arthritis.
Description — x-ray of knee with osteoarthritis — there are more than one hundred types of arthritis.
Managing osteoarthritis
There is no cure for osteoarthritis, but if managed effectively patients will still be able to enjoy a high quality of life. A patient should create a treatment plan with a general practitioner (GP).
Management options for osteoarthritis include:
An exercise program tailored to their condition and ability;
A weight management plan;
Manipulation and stretching of affected areas as well as the application of local heat or cold;
Pain management, including the use of medicines such as paracetamol or non-steroidal anti-inflammatory drugs (NSAIDs);
Mindfulness and meditation for pain management;
Devices such as braces, walking sticks, and shoe insoles; and
Joint replacement surgery, in the event of the failure of other therapies.
Exercise is a crucial part of any osteoarthritis management plan. Regular exercise has the potential to improve joint mobility and strength and reduce some of the symptoms caused by the condition.
Osteoarthritis prevention
© Maintain a healthy weight — excess weight presents a risk for osteoarthritis as a person’s weight-bearing joints are put under additional pressure;
© Control glucose levels — rsearch suggests that diabetes, which affects the body’s ability to regulate blood glucose, could be a significant risk factor for osteoarthritis;
© Diabetes can trigger inflammation which leads to cartilage loss — moderate exercise is a key way to keep joints healthy;
© As little as 30 minutes of exercise per day aids joint and muscle function;
© Rest — in the case of ligament tears and strains, dislocation and fractures, it is important to rest and recover properly;
© It is estimated that 50 per cent of people who experience a traumatic joint-related injury develop osteoarthritis — practice a healthy lifestyle; and
© This inclusive of diet (including drinking and smoking habits), sleep, stress management, and socialisation.
- Dr Isikeli is the clinical co-ordinator at Oceania Hospitals Pte Ltd.